The main weakness of the study was the lack of tumour characteristics beyond localisation and stage. A large study group enabled us to analyse long-term outcomes based on detailed subsites and stratified by TNM stages. The main strength of the study was the ability to use population-based nation-wide data collected uniformly over the study period. The unfavourable effect of advanced age decreased with higher stage. No survival differences between subsites were seen in stage II. In this population-based study, we found that the survival disadvantage of RCC patients was limited to those with hepatic flexure cancer in stage III, and those with ascending colon and hepatic flexure cancer in stage IV. The study protocol was approved by the Tallinn Medical Research Ethics Committee (decision no 2636, 14 February 2019). No other significant interactions were detected. As we found strong interactions between stage and all other variables, the EHRs are shown stratified by stage (because of small numbers, the results are not shown for stage I). Interactions between variables were tested with likelihood ratio test. The EHRs are presented with 95% confidence intervals (CI). Cases with unknown stage or unknown T category were excluded from the models. Lifetables for modelling were produced with the strs algorithm in STATA 14 (StataCorp, College Station, TX, USA).

Excess hazard ratios (EHR) of death within five years after diagnosis were estimated in the framework of generalised linear models using a Poisson assumption for the number of observed deaths for colon cancer subsites, adjusting for age, sex, period of diagnosis, and T category, based on complete analysis (2007–2016). The latter was calculated according to Ederer II method, based on national life tables, stratified by age, sex, and calendar year. Relative survival ratio (RSR) was calculated as the ratio of observed survival and expected survival of the underlying general population, based on complete analysis. In case of death or emigration, the respective dates were obtained. Follow-up for vital status from the date of diagnosis until 31 December 2016, was conducted by the ECR at the Estonian Population Registry using unique personal identification numbers. Cancer stage was coded into stage groupings according to UICC version 7 of the TNM classification. Percentage of microscopically verified cases was used as a data quality indicator. Cases located in the appendix (C18.1, n = 88) and other or overlapping sites (C18.8–18.9, n = 204) as well as death certificate only (DCO) cases ( n = 48) and cases diagnosed at autopsy ( n = 77) were excluded from the analysis (the proportions of DCO and autopsy were similar between the subsites).
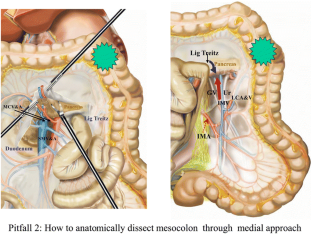
#HEPATIC FLEXTURE RESECTION CODE#
Subsites were classified as follows: caecum (ICD-10 code C18.0), ascending colon (C18.2), hepatic flexure (C18.3), transverse colon (C18.4), splenic flexure (C18.5), descending colon (C18.6), and sigmoid colon (C18.7). ECR is a population-based registry covering the whole country (1.3 million), it has data since 1968 and reporting is mandatory by law. The Estonian Cancer Registry (ECR) provided data on all adult (age ≥15 years) cases of colon cancer diagnosed in 2007 to 2016, regardless of cancer sequence. This study aimed to analyse possible survival differences between detailed subsites of colon cancer, accounting for TNM stage. The potential reason for this has been increased difficulty of laparoscopic lymph node dissection as well as the lower incidence of transverse colon cancer. Transverse colon cancer patients have been often excluded from trials examining long term outcomes between laparoscopic and open surgery. A Korean single-surgeon study described lower survival rates among ascending colon and hepatic flexure cancer.
A Norwegian prospective study reported reduced survival among transverse colon, splenic flexure, and descending colon cancer patients compared with other colon subsites. Nevertheless, information about the role of the more exact location of the tumour is limited. They also show differences in epidemiological features, sensitivity to chemotherapy, pattern of metastatic spread, and prognosis. RCC and LCC exhibit different mutations, molecular characteristics, and histology. The possible explanations for survival differences have been extensively discussed. Right and left segments of the colon have different embryologic origins with caecum, ascending colon, hepatic flexure, and transverse colon deriving from the midgut and splenic flexure, descending colon and sigmoid colon deriving from the hindgut. Several studies have demonstrated worse outcomes for right-sided colon cancer (RCC) compared with left-sided colon cancer (LCC).
